 By Matt Skoufalos
By Matt Skoufalos
For years, interventional radiology (IR) was “one of medicine’s best-kept secrets,” said Kris McVey, vice president of angiography at Siemens Healthineers; “more of a procedure service in the hospital basement.”
Nowadays, however, “that era is over,” McVey said, and interventional radiology (IR) has emerged as a “dynamic, front-line clinical specialty,” fundamentally re-engineering the era of value-based care. From stroke treatments to interventional oncology, what was once an interdisciplinary bridge between diagnostic imaging and minimally invasive surgery is projected to become a $4 billion global market in the next half-decade.
“[IR-driven] arterial therapies moved from salvage therapy to standard care for liver cancers, with adoption accelerating across the world,” McVey said. “Ablation expansion remains a cornerstone, and new energy modalities, like pulse-field ablation, are emerging to preserve the safety and precision of these procedures.”
The technology integration driving this procedural expansion requires more widespread installation of IR labs themselves as well as the education required to optimize their use. The increased complexity of the equipment and its associated training notwithstanding, IR technology supports “even more minimally invasive” practices, which offers several advantages.
“There’s an economic shift as healthcare moves from volume to value, and IR is the poster child,” McVey said. “Smaller incisions, faster recovery, lower cost, fewer complications; shorter or even no hospital stays.”
There’s not much to inhibit the future growth of IR with the exception of the capital investment required to establish, maintain and maximize its use. Those costs extend from the high-end, novel technology that forms the backbone of the IR lab to the work required to construct it.
“We’re doing a lot to transform the imaging suite into a precision cockpit that brings CT and angiography in the room together,” McVey said. “Now they’re bringing the ablation side to the imaging side, which is only going to enable us to have even more innovations and better integration of technologies.”
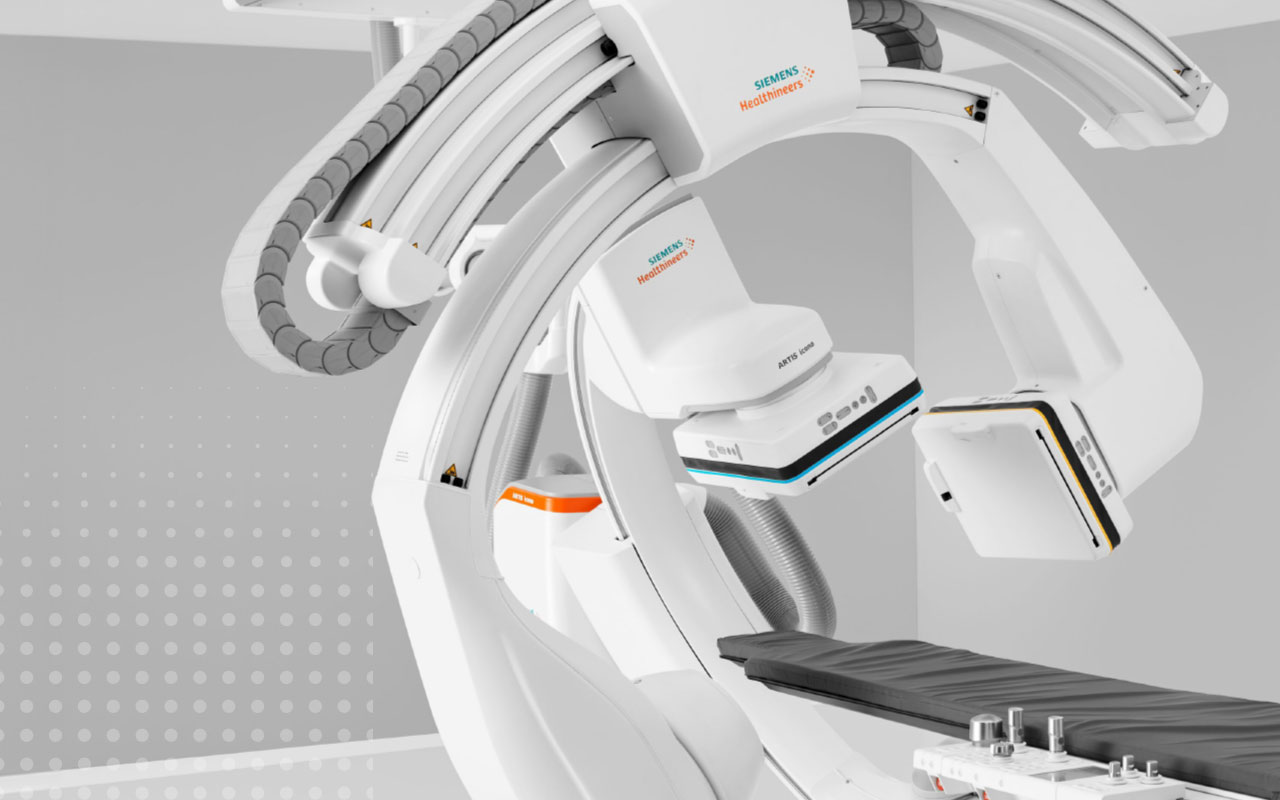
The latest generation of Siemens Healthineers technology in the Artis icono system reflects that approach to integrational imaging services: whether as a floor, ceiling, or biplane system, it is capable of supporting a variety of minimally invasive procedures.
“You can bring in different procedures to drive the utility of these labs,” McVey said. “With the biplane system of old, you can’t use the ceiling-mounted, lateral plane to do Dyna CT because it didn’t have the capability. Now you can take the lateral plane, travel it down the patient, and perform these procedures.”
Siemens Healthineers’ partnerships and acquisitions at the enterprise level help drive those technological integrations at the device level. Its 2021 purchase of Varian Medical unified their respective lab diagnostics, imaging and cancer treatment capabilities for a crossover audience.
Similarly, the 2023 Siemens Healthineers agreement with Atrium Health subsidiary IRCAD North America supported the development of a surgical research and experiential training center in Charlotte, North Carolina, that will help educate the next generation of IR practitioners. Both agreements have helped expand the capacity of its support for interventional radiology.
“The demand for these procedures is only going to get greater and greater, and the things we’re bringing into the technology to support demand are all going to need more physicians.” McVey said. “We’ve got to get people interested in moving into this field, getting the required education and going in this direction.”
From a practitioner perspective, Dan Shilo, director of Mt. Sinai West Interventional Radiology, and assistant professor at the Icahn School of Medicine at Mt. Sinai in New York, New York, believes that the most significant horizon interventional radiology will reach is that of an independent surgical subspecialty. The field has grown in that direction for more than a decade since the American Board of Medical Specialties granted it status as an independent medical specialty, and Shilo anticipates it will continue to progress in that direction as the complexity of IR care necessitates “more than a one-year fellowship to master and longitudinal patient relationships.”
Patients and referrers “want a disease process specialist, not a technician,” Shilo said, training clinical practitioners to open their own practices, or to join an existing department dedicated to their specialty, “which is better for patients and healthcare systems.”
“It’s a transition from a time when referrers would place an order for a procedure, an interventional radiologist would meet the patient for the first time in the procedure room, and then never see them again,” Shilo said.
 “That’s been the evolution, and those healthcare leaders that embrace this emerging IR practice model and the advantages that it provides are going to reap the rewards of this transformation,” he said. “Folks who want to stick to an antiquated IR practice model are going to be on the losing end of that landscape.”
“That’s been the evolution, and those healthcare leaders that embrace this emerging IR practice model and the advantages that it provides are going to reap the rewards of this transformation,” he said. “Folks who want to stick to an antiquated IR practice model are going to be on the losing end of that landscape.”
Transitioning interventional radiology to an independent, image-guided surgical subspecialty isn’t just want practitioners want, Shilo said, but also “what healthcare is now demanding.”
“On the academic side you’re seeing the emergence of interventional radiology departments in large medical centers that are independent from their diagnostic radiology counterparts,” he said. “This corresponds with an increasing number of independent IR practitioners operating in the community. They’re opening up their own complete clinical practices. People want agile, minimally invasive outpatient work. It’s absolutely a viable practice that someone can establish, and it’s great for patients and great for referrers in the community.”
The key mechanism, he said, is being “fully consultative on the disease process.”
“That’s where you can really provide the most impact for patients and referrers,” Shilo said. “They want somebody who takes complete ownership of the disease process and the patient, not someone who just hands it off to another subspecialty, or back to the referrer. Patients get better care in that model.”
Growing IR practices in the broader community can improve access to the therapeutic benefits of the technology it leverages, resolving what Shilo described as “massive unmet needs in the community for many diseases and minimally invasive therapies that IR can provide.” Even beyond addressing current patient demand, embracing interventional radiology is more about keeping pace with a shifting landscape rather than building capacity within an existing one, he said.
“Both patients and [healthcare] leaders are demanding minimally invasive procedures, rapid recovery, limited inpatient stays, and there’s no specialty better suited to provide that than IR,” Shilo said.
For image-guided proceduralists, the emergence of AI has only served to further the clinical role interventional radiology plays. Shilo pointed to the emergence of Pulmonary Embolism Response Teams (PERT) as akin to stroke teams in the delivery of rapid peri-procedural care, supported by the adoption of artificial intelligence technologies. Many current systems scan imaging as it’s performed, and alert practitioners immediately to intervene faster and deliver better-quality outcomes.
“How does a pulmonary embolism normally get diagnosed?” Shilo said. “A patient presents to the ER with a respiratory complaint, a CT scan is obtained to look for blood clots; the patient returns to the ER, then the ER waits for a report.”
“The diagnostic radiologist needs to get to it on their list, read the study, call someone in the ER about the finding, notify them of that finding, that ER provider then calls a consulting physician, and so on,” he said.
Instead, using an AI notification platform, Shilo and the IR team on the PERT are notified via an app and can immediately view the patient’s imaging, trend laboratory data, and hemodynamics via their electronic medical record.
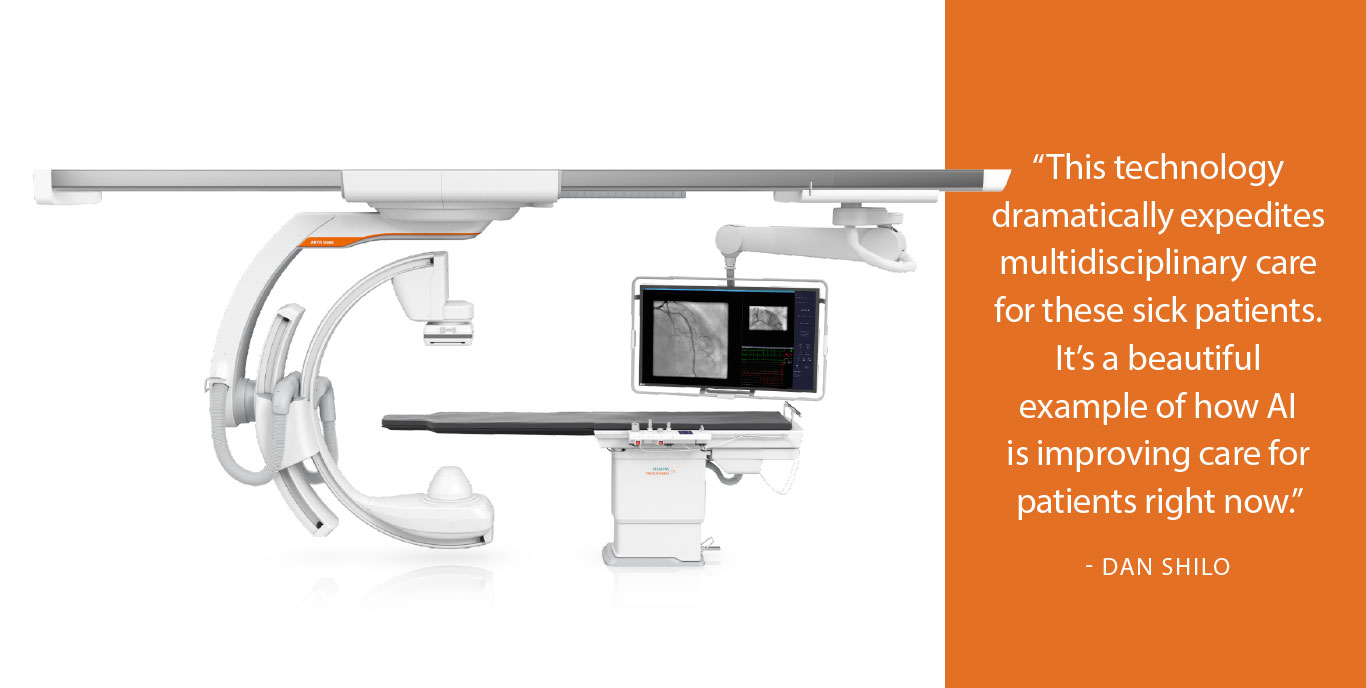
“I can risk stratify a patient for pulmonary reperfusion therapy while they’re still lying on the CT table, before the diagnostic radiologist on call is even aware of the scan,” Shilo said. “This technology dramatically expedites multidisciplinary care for these sick patients. It’s a beautiful example of how AI is improving care for patients right now.”
Even beyond the emergent setting, AI technologies are enhancing intraprocedural treatment delivery, Shilo said, noting that “multimodality integration across MRI, ultrasound, CT, and angiography in coordination with treatment confirmation software is allowing care to be delivered more precisely.”
The emerging use of surgical robotics in the IR space has the potential to expand access to minimally invasive interventional practices, even as diagnostic radiology continues to take a more distributed approach to care. Making use of professional talent where it’s located can help match patients with the best available care options, even if they’re not physically nearby.
“These robotic technologies are currently in their infancy, but we’ll one day get to a point where an interventional radiologist can control a robot remotely doing a procedure many miles away, if not halfway around the globe,” Shilo said. “That model may provide patients access to therapies that otherwise wouldn’t have been available to them, although the widespread commercial availability of that technology is many years away.”
“The paradox occurring right now is that there is an increasing interventional radiology clinical footprint, both in large academic centers and out in the community, whereas the diagnostic radiology footprint is increasingly remote,” he said.
Saher Sabri, M.D., is chief of interventional radiology at MedStar Health, professor of interventional radiology at MedStar Georgetown University Hospital, and president-elect of the Society of Interventional Radiology (SIR). Sabri underscored Shilo’s perspective that interventional radiology will continue to pave a path separate from diagnostic imaging, whether within the hospital or in independent practice.
“The model that has been pretty dominant – IR as part of a diagnostic radiology group – is going to start evolving,” Sabri said. “Many people will potentially leave such groups and either contract directly with the hospital, or join an IR group and contract with multiple hospitals.”
The majority of SIR members work in private-practice settings outside of the traditional academic centers, he said. Some are part of physician-led, diagnostic radiology groups; others are hospital-employed, which Sabri said is becoming a more popular model across all specialties as hospitals continue to consolidate. Other interventional radiologists practice out of outpatient labs or ambulatory surgery centers; they may own their own facility, participate in a group practice, or work in a private-equity model, as patients choose the setting in which they’re most comfortable to receive treatment.
“There’s a national shortage of interventional radiologists, and a lot of it has to do with diagnostic radiologists who [formerly] did minor interventional procedures, and now are working from home or imaging centers,” Sabri said. “They’ve left a void that is being filled by interventional radiologists, which gives them a chance to contract directly with hospitals.”
“The theme behind all of this is the clear delineation of the way we practice, and how it’s becoming significantly divergent from diagnostic radiology practice,” he said. “There’s a lot of focus on seeing patients and doing evaluation and management along with the procedure, which can vary in complexity.”
Sabri believes that interventional radiologists must continue to advocate for the specialty and the technology necessary “to do our job fully.” That coincides with the interests of hospitals that want to offer more and more IR procedures and are willing to acquire the equipment to facilitate them, the better to meet patients where they are and avoid transferring them out.
“We are equipment-heavy, but the goal is to have this equipment available to you to be able to provide the service that you need,” he said.
Providing minimally invasive care close to home is “well worth the investment,” Sabri said, because it’s a primary specialty that brings patients to the hospital. In addition, for surgery, orthopedics, oncology, gastroenterology, or transplantation, interventional radiology functions as a supportive clinical specialty; Sabri argues that “having IR is almost mandated.”
“I think it’s all about showing your value to the health system, so they know that having a robust interventional radiology service is better for the patient this system cares for,” he said.
Minimally invasive procedures facilitated by IR can decrease patient lengths of stay, which Sabri argued is “a major contributor to the hospital bottom line,” and so is more tightly integrating the IR practice in with other specialties so that other services advocate for it.
For example, Sabri pointed out that nearly half of all transplant patients have an IR procedure afterwards, and so the interventional radiology team is “fully integrated” with the transplant team “because they know that without us being successful, they can’t do what they do.” Similarly, IR can deliver nerve ablation that provides relief until a patient is ready for a knee replacement.
“We need all the robust prongs of treatment for us to maintain our patients in the system,” Sabri said. “They advocate for us as well as we advocate for them; for us to be successful, our specialties are successful as well.”
“All of that draws patients to the healthcare system,” Sabri said. “To have a successful connection with hospital leadership is to work hand-in-hand with our colleagues to show our value for them. If you are an integral part of a strategic service line, you’re integral to the health system.”
At the same time, Sabri said it’s important for interventional radiology to clearly define its relationship with diagnostic radiology. For all the benefits IR enjoys by being integrated with DR, “in certain settings, it can be something of a hindrance,” he said.
Amid the clinician shortage in diagnostic settings, a radiologist who is dual-certified in IR and DR may be asked to help fill roles in each setting, which can have the unintended consequence of undercutting the growth of a thriving IR practice.
“We’re adjusting the training pathway to match current practices,” Sabri said. “We have a lot of benefits of being aligned with diagnostic radiology, because this is where we started; this is where our big tent is. Eventually, maybe a training pathway could evolve to allow people to focus their practice to be more clinical, more procedural and less imaging.”



